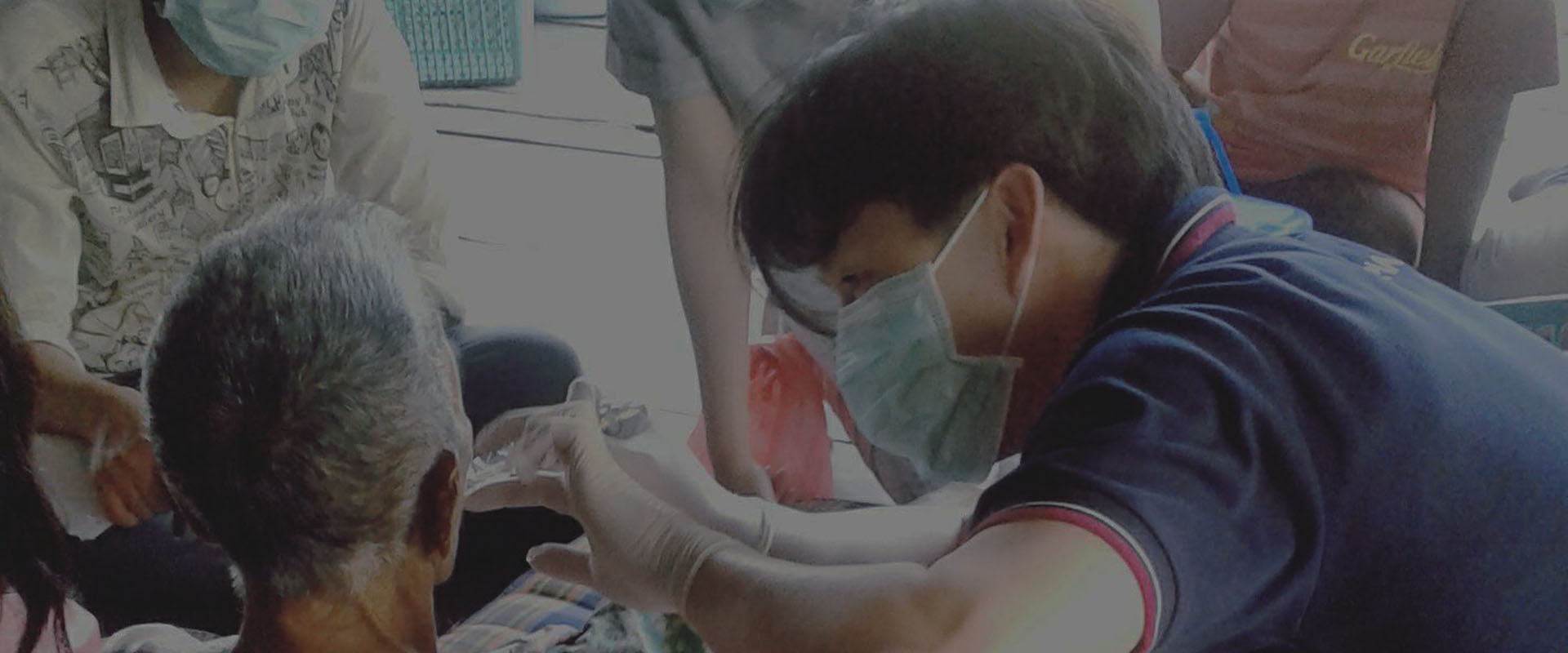
Story: Woraphong Wechamaleenonda
Dental hygiene may not seem that important to most people, because it does not usually create many problems in our daily life. It’s just cavities or wisdom teeth that may give us some trouble, but a quick visit to the dentist will take care of it. However, our mouths are actually more important than we think, because it is an excellent reflection of our general health. The signs of many health problems usually present through the smell, color and feeling of our mouths, and inversely, bad dental hygiene can transmit serious infection into the rest of the body, because the mouth is connected to many important organs such as the lungs, heart and cardiovascular system. Therefore, a good quality of life — when eating, speaking, smiling or laughing — can’t be lacking in good dental hygiene. This is especially true for the elderly, because aging greatly increases the risk of dental health problems as the general health of the body declines. Side effects from medication to treat various health conditions also mean that maintaining dental hygiene is different and more complex for the elderly. This has led to the development of a specialised field of medicine known as elderly dental care.
The History of Elderly Dental Care
Approaches to elderly dental care began to surface in Western countries around thirty years ago, as these were countries that had transitioned into an ageing society before countries in other regions of the world. Therefore, they were already encountering problems in elderly dental care, and were in the process of developing a body of knowledge and dental care systems, which evolved according to changes in social context. In the beginning, elderly dental care was not yet institutionalized: that is, if an elderly patient had become unable to travel to the clinic, or had moved into a nursing home, their relatives or nursing home staff may rely on their personal connection to a dentist, who may have been the patient’s regular dentist or a community dentist, and ask them to come give the patient a check up every once in a while if the patient is experiencing dental issues. Gradually, dentists and dental hygienists became a fixture of hospitals and nursing homes, as in the present.
Often, older people’s dental problems are mostly the result of the slow accumulation of issues from childhood to old age, such as gum disease, cavities and tooth wear. Part of it is the consequence of the body’s natural deterioration, but other factors include inadequate dental hygiene and the impact of side-effects from diseases, treatment or medication such dry mouth and saliva shortage, which increase the risk of cavities or severe gum infections that can cause teeth to fall out. They can also lead to cuts in the mouth, which can sting or make it difficult to swallow.
Traditionally, dentists are only taught to look after a patient’s dental hygiene, with an emphasis on treating ailments until they are completely cured — which isn’t adequate enough for elderly patients with complicated physical, emotional and social conditions. Dentists should be aware of the patient’s needs and quality of life, as well as their family’s. If the patient doesn’t feel ready for treatment, the dentist must find other alternatives to caring for them, or wait until the patient is ready for treatment without pressuring them.
As for elderly dental care policy in Thailand, the Ministry of Public Health has traditionally given more importance to children’s dental care, because they deem children a crucial segment of the population for national progress in the future. Since then, they have gradually given more consideration to elderly dental care once they recognized that Thailand was at the threshold of becoming an aging society, and directed their efforts towards the education system.
Dentists have incorporated elderly dental care into dental curriculum, and have sent people to study with elderly dental care experts in countries that are at the forefront of this field. Upon their return around ten years ago, they revised the Thai dental curriculum to match universal standards. They also worked with government organisations involved in public dental care, such as the Bureau for Dental Health, the Department of Health and the Dental Innovation Foundation, were building agencies directly responsible for elderly dental care, which evolved into the Elderly Dental Care Plan of Thailand. The plan includes the distribution of funds towards training dental care workers so that they are able to provide dental care to elderly patients with special needs: this encompasses patients with dementia, Parkinson’s, oral cancer, skin cancer on their face; patients with mobility issues from traumatic brain injury or cerebrovascular disease, as well as psychiatric, bedridden and end-stage patients.

Dental Care for Terminally-ill Patients
Terminally-ill patients are a segment of the elderly population. Most of the time, dentists are not usually part of the primary caregiving team, but usually become involved when the patient’s doctor or nurses request that they treat a patient’s dental issues. For example, they are asked to treat patients with cancer in their head or face, because both chemotherapy or radiation have consequences for dental health, giving patients dry mouth, inflammation and wounds, which lead to pain, discomfort or bleeding; wounds that smell. ICU patients have loose teeth that may fall into their throat, or grit their teeth until they have wounds on their lips and in their mouth. In the last stage of brain diseases when the mouth is coated with dry phlegm, if the mouth isn’t kept hydrated and clean, the patient will be in discomfort or at risk of choking on their saliva and phlegm. If the patient can still somewhat eat, dental ailments will make it difficult for them to do so. Dentists therefore play an important role in alleviating pain, hydrating the mouth, managing symptoms and ensuring that the patient is as comfortable as possible. They can also protect the patient from the danger of a fallen tooth, food residue or phlegm lodging in the throat.
Advocacy Work and Challenges
At present, dental care workers in the public sector account for half of all dentists in the country, and are mostly concentrated in Bangkok. They are not distributed enough to adequately care for citizens of every age group. Though training programs for dentists have been organised over the last 3-5 years, the development of a division of dentists who can look after elderly patients in practice, is still unable to keep up with the present circumstances. Important initiatives that helped develop a clear system of dental care training were the Elderly Dental Care Plan of Thailand for 2015-2022 and the allocation of a budget for training the capacities of dental workers on many levels: whether by sending a number of dental workers for further education abroad, the production of a body of knowledge and manuals on practicing elderly dental care, and most interestingly, training dental care workers to become key movers in creating dental care teams that treat elderly citizens in their designated area through a 4 month training program at the Department of Dentistry at 8 universities. Some curricula covered holistic healthcare: participants learned about approaches to long-term patient care and clinic design for the comfort elderly patients according to the foundations of a healing environment; participants also discussed lessons that aren’t covered by formal education from each others’ direct experiences in the field. A professor of dentistry and family physician gave advice on caregiving, listening to patients and communicating with patients. Participants were also given tools for their personal education, such as the “Life Unlock” card game, the Satir method of behavioral analysis and other techniques that most dentists do not study.
On top of that, family physician policy, or in other words, medical and public health primary care services that focus on multidisciplinary teamwork and work conjunction with other organisations through the District Committee for the Development of Quality of Life, which works in community-based healthcare, was pivotal to getting dentist to join forces with other healthcare professions such as nurses, physical therapists, practitioners of Thai traditional medicine. No longer bounded by the dental room, dentists also had the opportunity to become part of teams that visit elderly patients at their homes.
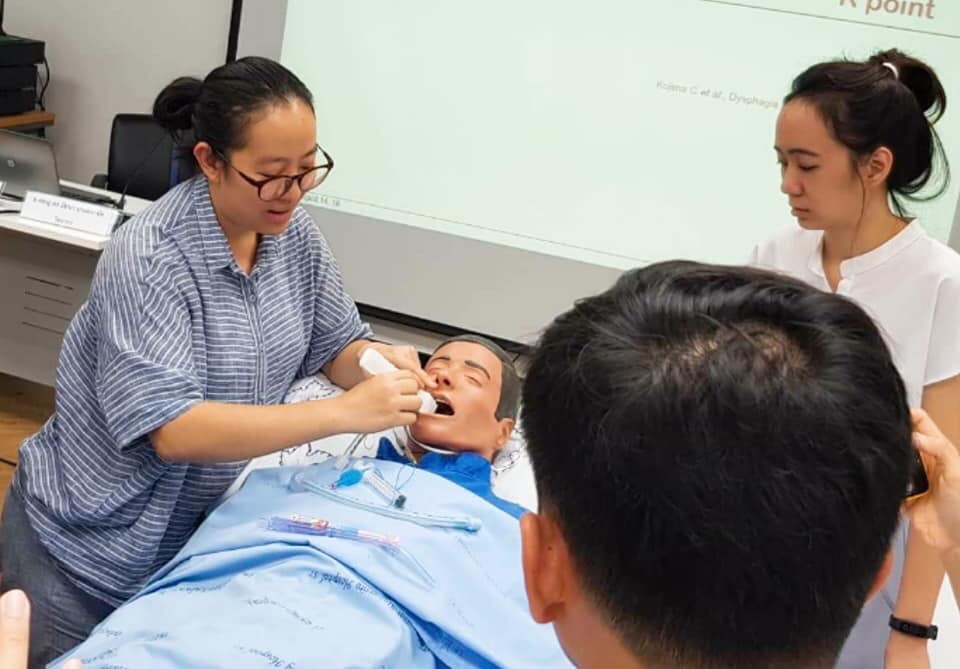
Though elderly dental care advocacy in Thailand has started to have direction and become more organised, there are still many challenges to face: addressing the extra burden shouldered by dentists who are caring for other demographic groups, maintaining momentum with child and maternal dental care, with the addition of dental care for the elderly and bedridden patients, which is still a new and difficult field. These factors make it difficult for dentists to allocate their time and with the demand of having to put new and unfamiliar knowledge into practice, some dentists still do not feel confident enough to treat patients that are bedridden or in critical condition.
There are also many structural problems, such as the gap between the Ministry of Health’s evaluation system and the reality and practice of caring for the eldelry. For example, the success of care is determined by the number of teeth in each elderly patient, regardless of whether the patient is healthy or in a dependent group. Furthermore, the evaluation system omits the functionality of the mouth and teeth, or the improvements made to a patient’s quality of life, in its analysis.
On the topic of the shortage of healthcare workers, there is also another profession, in addition to a lack of dentists, that is in short supply: dental nurses in Tambon Health Promotion Hospitals and public hospitals, who are an important workforce in the provision of dental healthcare for elderly members in the community. A major problem is that there has been very little progress in the dental nurse profession. There also issues with the allocation of dental nurses to hospitals. These are significant obstacles to the elderly dental care movement, with the shortage of dental nurses arising from the limitations of the current Dental Profession Act, which permits public dental workers to visit patients at their homes, but not dental workers in the private sector. As a result, the country suffers from no small lack of dental workers to look after elderly patients at home. Securing the participation of private sector dental workers in the future will definitely be one solution to the problem.
Lastly, insufficient access to necessary resources for elderly dental care, such as artificial saliva and high fluoride toothpaste — a gentle product that does sting or cause allergic reactions in elderly patients, helps control certain diseases and ensures that they feel comfortable when brushing their teeth — should not be overlooked too. Businesses import very small amounts of these products because most Thai dentists, due to a lack of awareness, do not use them at present. Therefore, when these products are needed, there are none available. Currently, Dr. Mantha Ketratat, a professor at Thammasat University’s Department of Dentistry, is studying the indispensability of these products to dental healthcare. She will use her findings to persuade businesses to increase their imports, and encourage local production of the products.
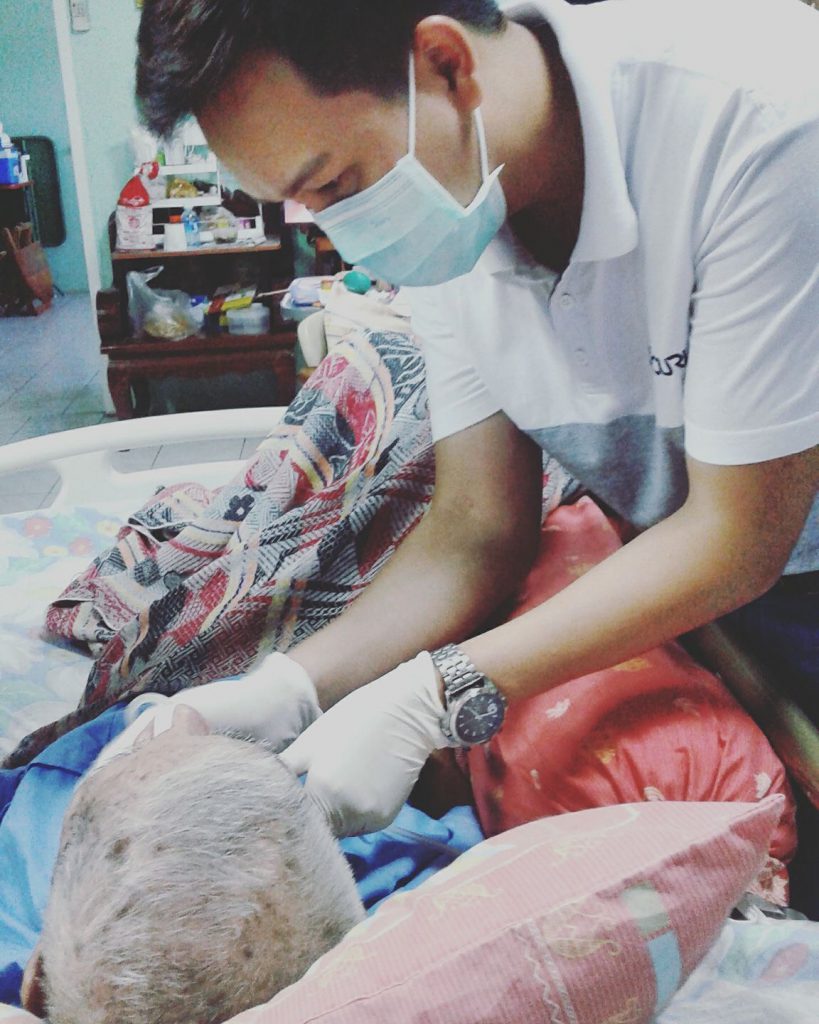
Looking After One Another Even in Old Age
As many parties join forces to make the products mentioned above more accessible, an array of useful initiatives for the elderly dental care movement are beginning to emerge that would enable patients and their families to look after themselves without needing to visit a hospital. For example, the Department of Dentistry at Thammasat University is in the process of creating a website for educating patients, their families and the public about personal dental care through easy-to-understand cartoons. They inform readers on what to do if a patient refuses to open their mouth for cleaning and how to choose the brush size and appropriate equipment for different contexts. It also carries advice and examples of successful patient care.
Another interesting initiative is designing the Masters Students’ Dental Clinic at Thammasat University to accommodate a restorative space for caregivers, since relatives usually sit and chat among themselves at the clinic while waiting for the patient. Organising activities for them while they wait, such as the “Life Unlock” card game, a game that fosters dialogue on life and death, allows them to self-reflect and perhaps better understand the patient. Professor Mantha observes that elderly patients’ relatives “sometimes release a flood of emotions after being asked a single question, as no one usually asks them how tired they are or what they go through in their daily life”. Accompanying their elderly relative to the dentist can be like meeting up with a friend to vent about their difficulties, which is another aspect to looking after one another.
This is the narrative behind one facet of preparing for Thailand’s transition into an aging society so that elderly citizens who have served the country for many years are cared for and not left behind in their old age.
Information and accompanying photographs:
Interview with Prof. Dr. Mantha Ketratat, Department of Dentistry, Thammasat University, Rangsit on 16/10/2018. Prof. Dr. Mantha Ketratat was the first dentist to graduate with a degree in elderly dental care abroad, before returning to community dentistry and elderly dental care at the Department of Dentistry, Thammasat University. She has constantly been a major force behind the efforts to raise awareness and organize around elderly dental care over the last ten years.